Is Meat Allergy Much More Common Than Expected?
London, UK - 1st March 2010, 12:05 GMT
Dear ATCA Open & Philanthropia Friends
[Please note that the views presented by individual contributors are not necessarily representative of the views of ATCA, which is neutral. ATCA conducts collective Socratic dialogue on global opportunities and threats.]
Severe allergic reaction to meat may not be rare. Eating meat may be a much more common trigger for anaphylaxis -- a severe and potentially fatal allergic reaction -- than previously thought. The findings were presented over the weekend at the American Academy of Allergy, Asthma & Immunology (AAAI) annual meeting in New Orleans. A person who suffers an anaphylactic reaction to something unknown is at increased risk of recurring anaphylaxis if the trigger isn't identified. Scientists appear to have found an answer for people who experience one of the most severe and life-threatening allergic reactions without knowing why.
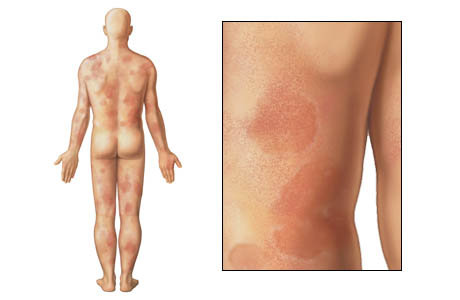 Severe Allergic Reaction
Severe Allergic Reaction
A sugar carbohydrate in meat called alpha-galactose may be the unrecognised cause of recurring severe allergic reactions in some patients, according to the study. The study included 60 people in Australia and the US who had unexplained extreme allergic reactions, anaphylaxis, with no known cause. Allergy tests revealed that 25 of the 60 patients had positive responses to alpha-gal. Scientists found immune system proteins called immunoglobulin E (IgE) antibodies in 25 out of the 60 patients who had unexplained allergic reactions.
Previous research had indicated that people who have the IgE response to alpha-gal experience anaphylaxis or hives three to six hours after consuming mammalian meat. Therefore a scientific team of investigators decided to explore how many cases of anaphylaxis of unknown cause may be triggered by eating meat.
Dr Scott Commins of the University of Virginia, who led the research, notes: We believe that the presence of IgE antibody to this sugar [alpha-gal] is wider spread in the human population as a whole than we had initially expected. What we are finding is that this traditional notion of allergy to meat being very rare may, in fact, not be true. Alpha-galactose is produced in most mammals but humans and great apes make an antibody to the sugar. So the problem becomes [manifest] when people make IgE antibody to this sugar. When they eat meat or dairy products that contain the sugar then they get a delayed reaction. The anaphylaxis may seem to appear out of the blue because the meat or dairy may have been eaten four to six hours earlier. The typical scenario has been if you don't react to food within two hours, then it's not the food, in this case that doesn't seem to be true. Previous research and the current study continue to suggest not only that IgE to a carbohydrate has important clinical implications in food allergy and anaphylaxis, but the presence of this antibody may well have been under appreciated in terms of the number of patients affected and geographical scope.
The tests did not identify any other allergens that would explain the cause of anaphylaxis in the 25 patients who were positive for alpha-gal or in the other 35 patients, the study authors noted. No other patterns were found.
According to the American Academy of Allergy, Asthma & Immunology (AAAI) approximately 3 million children younger than 18 years were reported to have a food or digestive allergy in the previous 12 months, and more than 3% of adults have one or more food allergies. The AAAI also notes that food allergies account for 35% to 50% of all cases of anaphylaxis, and that food allergies cause approximately 150 to 200 deaths per year, based on a 2003 study from the Mayo Clinic.
[ENDS]
We welcome your thoughts, observations and views. To reflect further on this subject and others, please respond within Twitter, Facebook and LinkedIn's ATCA Open and related discussion platform of HQR. Should you wish to connect directly with real time Twitter feeds, please click as appropriate:
. ATCA Open
. @G140
. mi2g Intelligence Unit
. Open HQR
. DK Matai
Best wishes

